The lay press has again questioned the role of “cholesterol” in the pathophysiology of atherosclerotic cardiovascular disease and the relative benefit of Statin therapy especially in healthy people with no heart disease. Chris Kresser writes an impressive blog:
The Diet-Heart Myth: Cholesterol and Saturated Fat Are Not the Enemy
By Chris Kresser on April 19, 2013
Professor Tim Noakes has supported this ethos with both authors slating the benefit of Statin for “primary prevention of cardiovascular disease” in so-called heathy people (I will address this in my next blog).
Both authors are spot on with their understanding that cardiovascular disease is a disease of lipoproteins and not cholesterol. Both authors are correct that 2/3 of people who eat diets low in carbohydrate but rich in cholesterol and saturated fat may actually improved their HDL and LDL particle size. One needs to point out though that 1/3 of people will severely deteriorate their lipogram and seriously increase atherogenic lipoproteins probably due to LDL-receptor defects and in these individuals their vascular risk is very high.
I agree therefore that we need to stop talking about cholesterol and cardiovascular risk but rather talk of the “atherogenic lipoproteins” and “total atherogenic risk”.
LDL-C or apoB as the Best Target for Reducing Cardiovascular Disease:
For more than 20 years, LDL-C has been considered to be a major lipid risk factor, and in most national guidelines, LDL-C is considered to be the main target of lipid-lowering therapy. Large meta-analyses (see later) of interventional studies with statins have shown that reduction of LDL-C leads to reduction of the risk of coronary heart disease (CHD) and CVD in people with established vascular disease (secondary prevention) and in healthy people (at risk) but with no vascular disease (primary prevention).
However, even persons subjected to an active therapy in these trials display a high residual risk. One of the reasons for such a high residual risk may be the fact that LDL-C is not necessarily the best risk marker in all individuals.
At present, obesity and obesity-related insulin resistance, metabolic syndrome and Type 2 diabetes mellitus (T2D) is a worldwide phenomenon. Even in patients with metabolic syndrome and diabetes, lipoproteins play the major role in the development of atherosclerotic macrovascular complications. However, LDL-C is not the major characteristic of lipid changes associated with the aforementioned states. These states are associated with atherogenic dyslipidemia, characterized especially by increased levels of triglycerides (TGs), reduced HDL-C and an increased prevalence of small dense LDL (sdLDL) at relatively normal levels of LDL-C. Low HDL-C and high plasma TGs are considered to represent an important residual risk besides LDL-C.
Nevertheless, normal LDL-C does not mean that the atherogenic particle number is normal, and this fact is often underestimated. The increased number of sdLDL associated with atherogenic dyslipidemia is reflected in increased concentrations of apoB, which is a better marker of atherogenic lipoprotein numbers than concentrations of LDL-C. In fact, apoB is a key component of atherogenic dyslipidemia, as will be discussed later.
Pathophysiology:
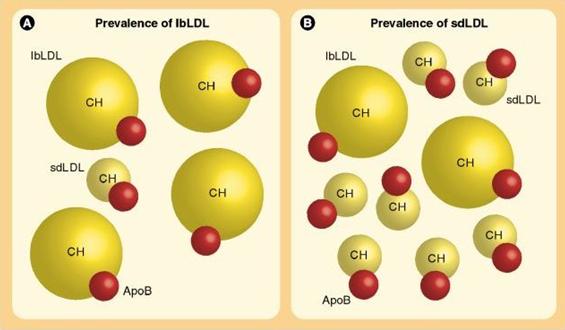
Atherogenic lipoprotein particles can vary considerably in their cholesterol content, but each particle contains only one molecule of apoB-100 (or simply apoB). As a result, serum concentration of apoB is a better marker of atherogenic lipoprotein particle numbers than both LDL-C and non-HDL-C (total cholesterol minus HDL). Especially in subjects with a large number of cholesterol-depleted sdLDL, LDL-C underestimates the number of LDL particles the most (see Figure below). Subjects with obesity, insulin resistance, metabolic syndrome, hypothyroidism; leaky gut syndrome and diabetes tend to have high levels of sdLDL and also have a multiplication of other potentially atherogenic lipoprotein particles rich in TGs, namely VLDL and their remnants IDL, which are not contained within the LDL-C parameter.
In the figure above the LDL-C level in specimen “A” and “B” may be equal but in “A” the lipoproteins are large non-dense fluffy with only 5 Apo-B (the red circles) compared to “B” where there are small dense LDL with other atherogenic lipoproteins with 9 Apo-B molecules.
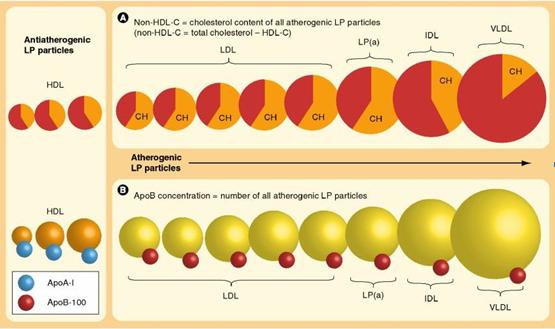
The concentration of apoB is better marker of the number of all potentially atherogenic particles because all these lipoprotein particles (VLDL, IDL, LDL [including sdLDL] and Lp[a]) contain only one molecule of apoB-100 and various amounts of cholesterol (see Figure below).
All apoB-containing lipoprotein species appear to be atherogenic to a greater or lesser extent, but larger apoB-carrying particles, such as VLDL, may be less atherogenic than the smaller LDL particles.
Small dense LDL particles are probably more atherogenic than large buoyant (fluffy) LDL as they enter the artery wall much more easily and are not well-recognized by LDL receptors and thus remain longer in the subendothelial space, where they undergo modification and induce inflammation. Modification affects the structure of apoB-100 so that it becomes a ligand for the scavenger receptors of monocytes or macrophages. Cholesterol then accumulates in the cytoplasm of macrophages to form foam cells, which is the characteristic feature of all stages of atherosclerosis.
Experimental studies demonstrated that apoB, by highly specific interaction with proteoglycans, leads to entrapment and retention of lipoprotein particles in the artery wall, where they become oxidized or otherwise modified. Thus, it is apoB and not the cholesterol content of the lipoprotein particle that leads to the initiation of atherosclerotic processes and subsequent deposition of cholesterol in the artery wall.
The greater atherogenicity of small dense (sd) LDL particles in comparison with large buoyant LDL is supported by findings from the Quebec Cardiovascular Study that confirmed that a greater proportion of sdLDL at baseline was a strong and independent predictor of CHD in the first 7 years of follow-up. By contrast, an elevated concentration of large LDL was a poor predictor of CHD in this study and seemed to be paradoxically associated with a low CVD.
Review of Prospective Studies Comparing apoB & LDL-C as Predictors of Cardiovascular Risk:
Numerous prospective studies have shown that apoB predicts CHD in both genders, and is better than LDL-C in this respect.The largest from these studies was the AMORIS, which observed 98,722 men and 76,831 women over the age of 60 years for approximately 5 years. In this study, by use of different multivariate analyses, apoB proved to be more significant than LDL-C and added predictive power to that of LDL-C for prediction of the risk of fatal heart attack.
Another major finding of the AMORIS was that in individuals with concentrations of LDL-C below the median, apoB was a better predictor of risk than LDL-C. This is a very important finding as almost 50% of coronary patients may have plasma cholesterol concentrations of less than 5.2 mmol/l and a large proportion of coronary patients with normal cholesterol levels have elevated apoB concentrations.
This finding can be explained by the presence of sdLDL and is in agreement with the results from the Québec Cardiovascular study,[ which showed that the risk of MI is higher in individuals who have high LDL-C and a high concentration of apoB than in those with high concentrations of LDL-C and low apoB.
A further important finding of the AMORIS is that apoB and apoA-I (the lipoprotein in HDL) added power to predict fatal MI not only in men and women under 70 years of age but also for those aged 70 years or more. Total cholesterol loses its predictive power in people aged 70 years or older, while apoB, apoA-I and the apoB:apoA-I ratio remain important risk predictors of MI in this age category.
Numerically, the steepest increase in risk of MI was obtained in the AMORIS for the apoB:apoA-I ratio, which increased approximately 3.8-fold in men and just below threefold in women when the risk for those in the highest quartile was compared with those in the lowest quartile.
Prospective studies support the concept that the number of atherogenic particles is a more important indicator of risk than the amount of cholesterol transported in these particles.
In which Populations does LDL-C most Underestimate the Number of Atherogenic Particles?
LDL-C most underestimates the number of atherogenic lipoprotein particles in conditions with a large prevalence of sdLDL. It was proved that sdLDL starts to increase with TG levels of 1.5 mmol/l. The increased number of sdLDL is particularly common in subjects with visceral obesity, metabolic syndrome and diabetes mellitus.
It is well-known that diabetes increases the risk of CVD more in women than in men. In particular, women who become diabetic differ from nondiabetic women in their markedly increased concentrations of apoB, while their LDL-C and non-HDL-C remain comparable with nondiabetic women.
Familial combined hyperlipidemia (FCH) also belongs to clinical entities associated with insulin resistance, an increased number of sdLDL and disproportionately increased concentration of apoB compared with LDL-C. Diagnosis of this most common familial dyslipidemia is based on measuring apoB and not just lipid. FCH is found in approximately 0.5–2% of the general population and in 10–20% of patients with premature vascular disease. In some cohorts of patients with a history of heart attack FCH was found in up to 40% of cases.
Small dense LDL is also frequently found in patients with established CVD especially in those with relatively low total cholesterol and LDL-C. In elderly people, LDL-C loses its predictive power while apoB still predicts the CHD risk. Approximately 45% of the population over 60 years of age have metabolic syndrome, which is characterized by an increased number of LDL particles at a relatively normal LDL-C concentration.
Thus, apoB measurement in order to assess CHD risk is especially important in the rapidly growing subset of the population with obesity, characteristics of metabolic syndrome, diabetes and in a growing subset of the older population.
Conclusion & Future Perspective:
It is usually argued that the introduction of apoB as a marker of risk and target of therapy would lead to confusion of both physicians and patients. For more than two decades, a great effort was devoted to education on the issue of the role of ‘bad cholesterol’ (LDL-C) in the development of atherosclerosis and the necessity of cholesterol-lowering therapy in the prevention of CVD. Thus, most authorities in this field think that it is necessary, at least for an interim period of time, to introduce apoB assessment to the routine lipid profile.
ApoB is a marker of the risk of atherogenic particles, especially LDL risk, and cannot substitute the whole lipid profile, especially at baseline examination. Thus, as this article suggests, apoB should be a part of the routine lipid panel at baseline. However, when apoB is the target, total cholesterol, LDL-C and non-HDL-C need not be measured on routine follow-up visits. Thus, apoB could unify all lipid targets representing the proatherogenic lipoprotein particle risk into one parameter.
Estimation of baseline TGs is useful, as a mild-to-moderate increase in TGs is a good marker of insulin resistance and its associated risk factors and also as a marker of increased risk of CVD.Even in patients treated with statins to achieve very low levels of LDL-C of less than 1.8 mmol/l, high TG levels represent a considerable residual risk.
Nevertheless, especially in hypertriglyceridemia, CVD risk is influenced by concomitant apoB levels. High apoB levels in hypertriglyceridemia indicate an increase in potentially atherogenic particles such as sdLDL and smaller TG-rich particles, such as IDL and smaller VLDL, while low apoB levels instead indicate an increase in larger TG-rich lipoprotein species such as chylomicrons and large VLDLs, which are less atherogenic (owing to their volume, they do not easily enter the artery wall). Thus, increased TG levels of ≥1.7 mmol/l are markers of increased cardiovascular risk.
Estimation of HDL-C is also important for the evaluation of CVD risk, as it is an independent risk factor for CVD. Even in patients treated with statins to achieve very low levels of LDL-C of less than 1.8 mmol/l, low HDL-C significantly contributed to macrovascular risk.
The research in recent years has shown that the functionality of HDL and its specific subpopulations may be even more important than HDL-C levels. Nevertheless, at present, we do not have a useful method for measuring HDL functionality in clinical practice. Various drugs can influence different HDL species and various HDL functions. Thus, the results of clinical end point trials and not HDL-C levels should be decisive in this respect. However, as most drugs used for the treatment of lipid disorders usually influence more than one lipoprotein class, it will be very difficult to decide which part of the outcome is an HDL-related effect.
Several observations have shown that for many antiatherogenic roles of HDL, apoA-I is more important than HDL particle cholesterol content. Thus, in future, HDL-C assessment could probably be substituted with apoA-I assessment until better methods for the evaluation of HDL functionality are developed.
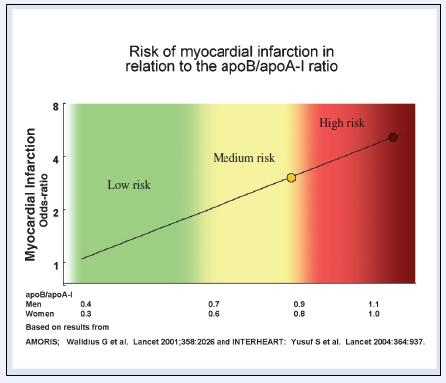
At present, the apoB:apoA-I ratio seems to be the best marker of cholesterol balance. It was shown to be the best marker of cardiovascular risk for MI and CVD in the AMORIS (see figure) and INTERHEART studies. I personally use the apoB:apoA-I ratio as a promising marker of both risk and treatment effect.
I keep my personal ApoB/ ApoA1 at 0.26 which as you can see from the figure above gives me an extremely low risk for AMI.
Summary:
- Recent data demonstrate that apoB is a better marker of risk than LDL-C and a more appropriate target of lipid-lowering therapy, especially in the growing subset of the population with established vascular disease, obesity, metabolic syndrome and/or diabetes.
Pathophysiology:
- As all potentially atherogenic lipoprotein particles contain only one molecule of apoB and various amounts of cholesterol, the concentration of apoB is a better marker of atherogenic particle numbers than LDL-C and non-HDL-C. LDL-C most underestimates the risk in subjects with an increased number of cholesterol-depleted small dense LDL. The number of atherogenic particles that are able to enter the artery wall is more important than the cholesterol transported in these particles.
Prospective epidemiological studies:
- In most of the available prospective studies comparing apoB with LDL-C and/or non-HDL-C, apoB is a better marker of vascular disease risk.
Interventional studies:
- Statins lower LDL-C and non-HDL-C more than apoB (in terms of percentage decrease from baseline and lower population percentile levels). Many patients reaching their LDL-C and non-HDL-C goals remain at high risk owing to high levels of atherogenic particles as judged by apoB assessment, especially those with elevated triglycerides such as those with metabolic syndrome and Type 2 diabetes. Owing to this fact, apoB provides a more consistent goal for lipid-lowering treatment and a better assessment of on-treatment residual risk than LDL-C and non-HDL-C.
Availability of apoB measurement & standardization
- The measurement of apoB is standardized, automated, inexpensive and does not require fasting samples.
Conclusion & future perspective
- ApoB should be measured in all subjects with abnormal lipid profiles and with a moderate or high risk of cardiovascular disease to evaluate their lipid-associated risk. ApoB should be the primary target of lipid-altering therapy. For the interim period of time, apoB should be measured as an additional and equivalent part of the lipid profile, at least in patients with a high cardiometabolic risk.
- The apoB:apoA-I ratio is a promising future parameter for evaluating both risk and treatment effects. ApoB and apoA-I should be measured in all prospective and interventional studies to obtain further evidence on this topic and to help to set appropriate targets.
- The ‘apoB paradigm’ should be explored in more detail as it offers new strategies for LDL-C lowering.
Cardiologydoc